Lichen Planus
Below you will find a selection of clinical images portraying Lichen Planus
1
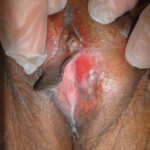
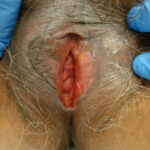
Lichen Planus with glazed erythema on left side of introitus with unilateral scarring. There is loss of the left labium minus. A vaginal examination is necessary to assess for vaginal involvement and scarring.
4
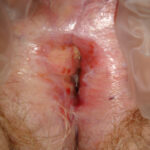
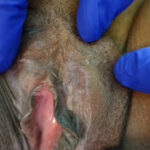
Here there is a mixed picture of erosive LP and Lichen Sclerosus. This patient requires biopsies to exclude VIN.
7
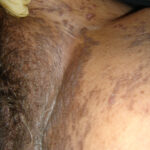
This is typical, classical LP with violaceous flat-topped papules with reticulations on top (Wickham Striae). This often leaves temporary post inflammatory pigmentation (brown). Self-limiting.
10
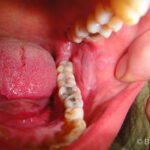
White plaque on buccal mucosa with lacy changes typical of LP. Plaques may sometimes erode. Also, check the tongue and gingival mucosa. Ask about swallowing difficulties (oesophageal LP).
2
Classical LP also termed Papulosquamous LP. Lacy white changes are observed. This type of LP is usually self limiting and is treated with topical steroid for a few weeks. Long term follow up is not necessary.
5
There is erythema extending into the vagina. This patient will probably require vaginal examination and treatment with intravaginal steroids plus dilators to prevent scarring.
8
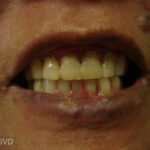
Pallor of lower lip due to LP. This patient would need a biopsy to exclude dysplasia as there is some scale/hyperkeratosis. Actinic (solar) damage can present in this way.
11
Reticulated pallor. There is suspicion of hyperkeratosis on the left side so a biopsy may be required for diagnosis.
3
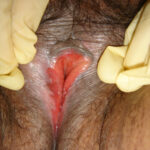
Erosive LP is also known as mucosal LP which may be a better term as erosive LP is not always erosive. However, there are erosions in this case. There is considerable architectural change with midline fusion and blunting of the labia minora. Topical oestrogen should be considered as there is pallor below the clitoris which is typical of peri or post menopausal changes.
6
There are erosions around the introitus arising on a background of pallor typical of LS. Lichen Sclerosus may progress to Lichen Planus or the two conditions may present together. LS and LP may represent a spectrum of disease.
9
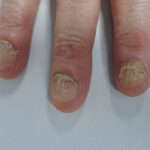
Extensive nail LP showing destruction of the nail plate and rough nails. Involvement of all 10 digits is the norm.